Major Considerations
General Anatomy and Function
The spine or spinal column (commonly called the backbone) is that part of the skeleton that runs from the skull above to the pelvis below. It is divided into five regions from top to bottom: the cervical spine in the neck, the thoracic spine corresponding to where the ribs arise, the lumbar spine in the low back, the sacrum at the base of the column and in between the two halves of the pelvis, and the coccyx hanging off the end of the sacrum (essentially all that remains in humans of what would be a tail in other species).
The spinal column is made up of a number of individual bones called vertebra which stack up one on top of the other and are joined together by ligaments, muscles, and a specialised cartilage called the intervertebral disc. The disc functions to tether one vertebra to the next but also as a shock absorber for the motion that occurs between neighbouring bones. Each vertebra has a large hole in its middle which, when joined up with that of the neighbouring vertebrae, together form a tube up and down the spinal column which is called the spinal canal.
There are usually seven vertebrae in the cervical spine, twelve in the thoracic, and five in the lumbar region. Those in the sacrum have fused together so that the original five here form one complete bone. The coccyx is rudimentary in humans and can consist of three to five bones. There can be some variations of “normal” here with so-called “segmentation anomalies” (for example, the top sacral vertebra may not be joined to the rest giving the appearance of six lumbar vertebrae). The presence of a segmentation anomaly is of no functional concern to an individual patient other than that the treating surgeon needs to recognise it when making certain diagnoses and planning treatment.
Looking from the front the normal human spine is usually very straight, although looking from the side there are three broad curves with the cervical spine in the neck being curved gently backwards (so called “lordosis”), the thoracic spine curved forwards (“kyphosis”), and the lumbar spine again curved backwards into lordosis. These curves balance each other out so that in the young adult spine the skull is position vertically over the pelvis. With aging we commonly see the head seeming to creep forward in front of the pelvis often due to “loss of lordosis” in the cervical or lumbar regions or “exaggerated kyphosis” in the thoracic spine. Although this can be a normal part of aging certain diseases, injuries, or degenerative process may lead to abnormal curves resulting in “loss of spinal balance” that may require treatment.
The pattern of vertebrae and intervertebral discs repeats throughout the vertebral column with each vertebra being named by region and number. The first vertebra in the lumbar region therefore is called “L1”, the fifth in the thoracic region T5, the third in the cervical region C3, and so on. Each intervertebral disc is named by reference to its two vertebral neighbours, so that the disc in between L4 and L5 is called the L4/5 disc, that in between L5 and S1 is called the L5/S1 disc (or less commonly the “lumbosacral disc”), that between C6 and C7 the C6/7 disc, etc. Since the sacrum is one complete bone there are no sacral discs, and the top two vertebrae in the neck (C1 and C2) are also very specialised to allow the high degree of movement between head and neck so that there are no discs here either. The highest disc level therefore is the C2/3 disc connecting C2 to C3, and the lowest is the lumbosacral disc at L5/S1.

Between each pair of vertebrae a spinal nerve (also called the nerve root) will exit from the spinal column. These are named from top to bottom so that the C1 nerve is the first to leave below the skull and above C1, then C2 coming out above C2, the C3 nerve above the C3 vertebra, etc. Things change a little at the junction between the cervical and thoracic spine at the base of the neck with the C7 nerve exiting above C7 as usual but then the C8 nerve coming out below the C7 vertebra (there are only seven bones but eight nerves in the cervical spinal column). The pattern is then consistent down the rest of the spine with each nerve leaving below its equally named vertebra so that the T1 nerve comes out below T1, T2 below T2, and so on all the way down to and through the sacrum. A spinal segment corresponding to one vertebra, its neighbour, their intervening intervertebral disc and the exiting spinal nerve is known as a spinal “level”.
Each spinal nerve will eventually look after a specific region of the body. That area where it supplies sensation is referred to as a “dermatome”, whereas that region where it controls muscle movement or motor control is called a “myotome”. Some of the spinal nerves (although not all) will also supply the so-called deep tendon reflexes such as the knee jerk reflex that a doctor may try to elicit with a tendon hammer. The importance here is that with careful assessment of sensory, motor, and reflex symptoms and signs the neurosurgeon can often identify which spinal level may be the site of a problem.
Dr Brennan is highly trained and experienced in the surgical treatment of conditions of the spine including spine tumours
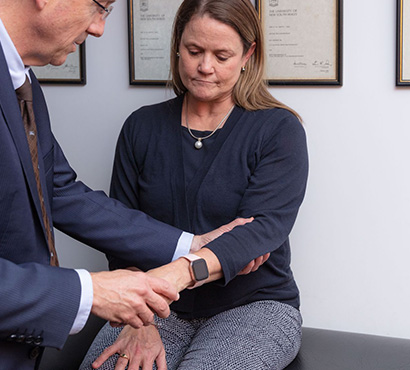
Common conditions throughout the spine
Herniated Intervertebral Disc
The intervertebral discs are the specialised cartilages that sit between two neighbouring vertebral bones. They function both as ligaments to help regulate the movement of one bone on the other, and also as shock absorbers that help to spread the load of the body weight in the upright human posture. Like all cartilages in the body they are prone to wear and tear degenerative changes (part of spondylosis) and also to true injuries.
A disc is said to herniate if the tough outer lining of the disc develops a tear that allows some of the softer inner component to “prolapse” or “slip” out. Sometimes this may just be a general bulge or on other occasions may be a free or so-called “sequestered” fragment. Often, this may cause little to no symptoms, but should the disc compress the underlying nerve or spinal cord it causes significant pain and loss of function.
Over time the body can heal disc herniations spontaneously, although not always. Initial treatments therefore are usually non-surgical in order to try and foster this healing process such as physical therapies, medications, injections, or just managing and allowing time to pass. If the condition is not improving or if there is evidence of worsening pain or loss of function, then surgery may be required to remove the herniated portion of the disc in order to decompress the underlying nerve tissue.
Spondylosis
This is the name given to the age related wear and tear changes that occur in the spine. It is not truly a disease since it will happen to everyone who lives into adult life, similar to going grey of the hair and developing ageing of the skin. It involves a combination drying out of cartilages, adjacent bony spur formation, discs becoming collapsed and bulging, ligaments losing their elasticity and seeming to thicken, sometimes degenerative cyst formation, and joints becoming unstable and incompetent. It is very similar to degenerative arthritis elsewhere in the body such as osteoarthritis. From person to person it can occur at different rates and at different ages related to genetic factors, heredity, previous injuries, and other conditions that may load the spine such as carrying around too much body weight, repetitive lifting and twisting movements over the years (e.g. so-called “builders’ or nurses’ back”), etc.
Where it differs from arthritis elsewhere however is that the combination of these changes can result in extra tissue being laid down which can then take up the space that is needed for either the spinal cord or the spinal nerves. This narrowing of the spinal space is what is referred to as “spinal stenosis”.
Since spondylosis itself is not a disease there is no definite treatment, and generally it is recommended to look to modify risk factors to try and reduce the rate that it progresses (e.g. weight reduction, identification and correction of errors of posture, avoiding wherever possible repetitive lifting and twisting manoeuvres, and core strengthening exercises).
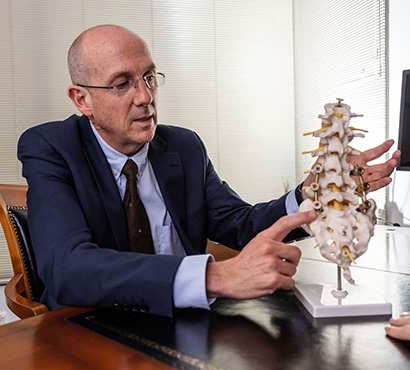
However, if spondylosis occurs to too great a degree and the extent of the stenosis is enough to jam the nerves or the spinal cord then it can lead to the conditions of spondylotic radiculopathy (if one nerve is jammed), neurogenic claudication (if many nerves are jammed particularly in the lumbar spine), and spondylotic myelopathy (if the spinal cord itself is jammed particularly in the neck).
The Spinal Canal and Spinal Canal Stenosis
The spinal canal is the name given to the roughly tubular space that runs up and down the centre of the spinal column and through which run the spinal cord, the spinal nerves and their coverings (including the cerebrospinal fluid or CSF). It is created by each individual vertebra bone having a large hole behind its weight bearing part (or vertebral body). With each vertebra lining up one on top of the other (separated by the intervertebral discs) this large central hole connects up to its neighbour and so forms a canal along the length of the spine.
The width and shape of the spinal canal varies from person to person in a normal way similar to other physical features such as body shape and height. If the spinal canal is on the narrow side of normal we sometimes refer to this as the person having a “congenitally narrow spinal canal”. Although this is not a problem in itself it can set the scene for potential nerve or spinal cord compression in the future as the canal develops further narrowing with age due to the process of spondylosis (described above). The combination of acquired or so-called spondylotic spinal canal stenosis on the background of a congenitally narrow spinal canal may well be something that brings a patient to the attention of a neurosurgeon. Although everyone will develop some degree of spondylosis and canal narrowing over time those of us with a wide canal to begin with may never get enough narrowing over the course of their life to develop nerve or spinal cord compression.
The spinal cord occupies roughly the top two thirds of the spinal canal, finishing at roughly the L1 level in most people. In the low back therefore there is no longer any spinal cord and the canal is occupied by all of the spinal nerves running down to exit at each level on their way to various parts of the leg and pelvis. These nerves together are sometimes called the “cauda equina” since they reminded the early anatomists of the hairs on a horse’s tail.
In the lumbar spine the canal become more triangular in shape, and in some people may even adopt a little clover leaf or “trefoil” shape. The side part or the arm of the triangle is referred to as the “lateral recess” of the spinal canal.
At the junction between each vertebra (a so-called “level”) a spinal nerve will travel out of the spinal canal through its own hole into the body on its way to look after a specific area (generally part of the arm for the cervical nerves in the neck, the trunk for the thoracic nerves in the middle back, and the leg and pelvis for the lumbar and sacral nerves in the low back and tail bone). These individual holes are called the “nerve root exit foraminae”.
All of these areas are prone to develop the process of spondylosis which can lead to extra thickened tissue being deposited over time. This may occur to such an extent that these spaces can become narrow leading to the description of spondylotic spinal canal stenosis. You may hear terms like “central spinal canal stenosis”, “lateral recess stenosis”, or “foraminal stenosis” referring to narrowing of these specific sites in the spinal canal which can have implication as to which if any of the nerves or the spinal cord may become compressed. The lateral recess is particular prone to stenosis since its roof is formed by large joints called facet joints which allow one vertebra to move on top of another. These joints are common sites of the wear and tear type changes that can result in the bony spurs, degenerative cysts, or thickened ligaments can make up the process of spondylosis. Since a spinal nerve often runs down through the lateral recess on its way into its own exit foramen this is a common site where nerve entrapment may occur.
Risk factor modification and preventative measures
Although the condition of spondylosis is in part an unavoidable aging process of the spine that will occur in all of us there are some risk factors which are generally understood to contribute to the extent and speed at which it develops. Some of these risk factors are beyond our control such as genetic predisposition, hereditary conditions, the suffering of previous injuries, etc. Research on stem cell therapy offers some hope that in the future some of these issues may be able to be addressed.
However, other risk factors are potentially able to be modified now to reduce the impact of spondylosis and, if you like, ensure your spine will last as long as you do. Broadly these risk factors include:
Giving up smoking – smoking “ages” the body tissues prematurely which is one reason why long term smoking can lead to grey, wrinkly skin and listless hair etc. In the spine this may aggravate the dehydration and breakdown of the discs and cartilages.
Identification and correction of errors or posture – how we sit, stand, and position our necks and backs during activities and work can over the years lead to “hot spots” of degenerative changes that may become symptomatic. Avoiding these postural errors may help reduce the extent to which these form.
Reducing weight and keeping weight down – in a common sense way the heavier we are the more load and stress there is across the spine as we go about our day in the upright position. Even when sitting down and seemingly resting our spine is working to support our bodies against gravity. Cartilage and disc wearing occurs as a direct response to the day by day and year by year loading that occurs based on our unique upright human physiology. Avoiding or reducing excessive weight gain can reduce these forces over time.
Avoiding wherever possible “injury prone activities” – this is particularly the case for the lumbar spine where the discs can be exposed to significant torsional loading moments in activities that involve repetitive bending, lifting, and twisting movements. These can be amplified in those activities that involve a lift, twist, and put down type action across the spine. Over time this may lead to so-called “micro-injuries” in the discs resulting in tears and sometimes frank herniations.
Core strengthening exercises – bones, cartilages, and ligaments will to some degree always wear down over time. However, with exercise we can maintain the strength in our muscles to help off load the forces that our spines are exposed during day to day activities. The so-called “core muscles” are those in the back and neck itself and also in the trunk generally such as the stomach muscles which, among other things, function to help spread the load that occurs through our spine and trunk as we go about our lives. The stronger they are the more that can be done with safety. Conversely, if core strength is allowed to lapse then all of the forces that occur must be met by the spine alone and hence it is more likely to suffer wear and tear injuries. In a very real sense therefore it is important to put the effort in to age well. Nonetheless, exercise carries the risk of injury and so it is worthwhile speaking to a physiotherapist or exercise physiologist to ensure that the these exercises are being down in an appropriate way for your individual case and with proper technique (a small error in technique for example may have the unwanted consequence of an injury prone activity as described above).
It can sometimes be helpful to remember that our spine evolved over hundreds of millions of years and became a major point of difference between humans and other mammals allowing us to walk around in an upright position. Furthermore, evolutionary anatomy teaches us that we separated from our closest primate cousins (chimpanzees) roughly 6 million years ago with our ancestors leaving the forests and becoming long distance runners on the African savannah. Modern humans started life in this habitat perhaps 700 thousand years ago. However, in only the last few hundred years we have developed an increasingly sedentary life style with even the most active of us still somewhat more stationary than our evolutionary forebears. A great deal of the trouble that people can experience in their spines comes from this mismatch between what our bodies evolved to do and what we actually do. Many measures aimed to improve spinal health come about by recognising this difference and trying to minimise it by becoming less sedentary and more active.
Axial Spinal Pain (low back pain and neck pain)
Spinal pain and particularly low back pain is a very common problem with as many as seventy percent of the adult population likely to experience at least one episode of significant low back pain in their lives. For most this is a self limiting problem that gets better, and as such it is so common that it can almost be considered as part of life in modern human societies rather than a sign of something going wrong. For others however it can persist or and become a chronic and disabling condition that may prevent normal activities and work, and yet others may be prone to multiple flare ups over their life in an on again off again pattern.
The initial treatment of acute low back pain usually involves a period of rest with simple pain killers (such as paracetamol or anti-inflammatories) followed by gentle mobilisation and physical therapies. Physiotherapy, osteopathy, chiropractic therapy, and various combinations of these can be tried together with other alternative strategies such as acupuncture. Stronger medications carry very real risks of dependence and aggravating the pain system in the body and so generally need to be avoided.
Medical therapies usually revolve around rehabilitation programmes, exercise related treatment, and core strengthening training. There can sometimes be a role for injection based therapy (e.g. cortisone injections).
The fact that there are so many treatment options that get tried for low back pain highlights one of the main dilemmas in this condition, i.e. the difficulty in diagnosing the underlying cause of the pain and the lack of knowledge in medicine as to the correct treatment. Even modern test such as MRI and nuclear scans may not reliably show the exact generator of the pain and often get mis-interpreted in this “grey area” of medicine.
Nonetheless, for pain that is persisting despite initial treatment, pain that is getting worse with unusual features (such as waking someone at night), or pain that has any flavour of nerve compression such as spreading down the legs an MRI is usually required to exclude identifiable causes such as nerve compression, fractures, deformity, tumours, etc. If these conditions are excluded however the MRI may not be able to show the underlying cause of pain in axial spinal low back pain.
Surgery therefore has a somewhat guarded and controversial role in treating this condition. Even experienced spine surgeons may hold divided opinions as to how effective surgery may or may not be in trying to treat low back pain alone. It requires a nuanced and careful assessment of the case, and sometimes the best thing a surgeon can do is to advise where surgery is just not a good option.



