Cervical Spine Surgery
Microdiscectomy
This is a minimally invasive procedure that allows decompression of a nerve in the spine that has become jammed by a herniated disc. A small incision is made in the back of the neck to enable a corridor to be created between the muscles and the spine and then a small window into the spinal column itself (via what we call a laminotomy). This then allows the nerve to be seen and the disc fragment removed. If the situation is one where the nerve is jammed by bony spurs (foraminal stenosis) the procedure involves a general widening of the funnel shaped nerve hole into a more open roofed cylinder shape so that the nerve has room. An operating microscope is used to allow this microsurgery to be performed. Xrays are used in the procedure to allow precision and accuracy.
Most patients can expect to stay one night in hospital, roughly one week where they can take care of themselves at home but not doing anything heavy (i.e. no vacuuming, bed linens, gardening, or carrying more than 3 kg), and roughly one month gradually increasing back to normal activities in a common sense fashion.
Return to desk work is usually within the first one to two weeks although more physical work should be delayed until four to six weeks to make sure that enough healing has occurred before the spine is loaded.
When properly assessed beforehand this treatment option can be very helpful at relieving the symptoms of radiculopathy if they are not settling with non-surgical treatments.
Dr Brennan is highly trained and experienced in the surgical treatment of conditions of the spine including spine tumours
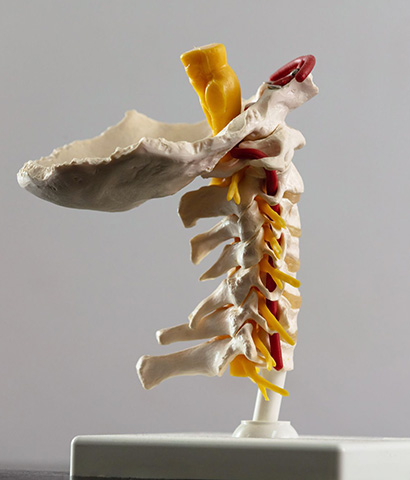
Posterior Cervical Foraminotomy
This procedure is performed to decompress a nerve that has become jammed by arthritic spurs due to spondylosis. It is similar to a microdiscectomy (explained above) except that goal is to generally widen the nerve exit hole and clear away overgrown spurs to create space for the nerve.
In the neck where the exit hole is somewhat funnel shaped this procedure converts this shape into a more open roofed cylinder and hence allows the nerve room to gently bow out of the spinal canal on its course into the neck and eventually the arm.
Recovery from this procedure is often identical to that for microdiscectomy.
Cervical Laminectomy
This operation is performed via an incision on the back of the neck designed to allow the removal of a portion of the bone at the back of the spinal canal (called the “lamina” of the vertebral bone) in order to unroof the space for the nerves or spinal cord. This increases the size of the spinal canal thereby decompress these structures. The amount of bone removed needs to be tailored to the individual situation so that enough space is created for the delicate neural elements. The guiding principal is to limit this to the minimum required. Some patients may be surprised to learn that the human body can safely function even without this part of the spinal bone, but it has been well shown over many decades that this is the case and so laminectomy in one form or another remains a very common procedure in the treatment of spinal conditions occurring within the spinal canal.
In some situations it may be necessary to supplement a laminectomy with a posterior spinal fusion in order to reconstruct the spine, correct deformities, or prevent further deformity in the future.
This operation is most often used to treat cervical spondylotic myelopathy when the spinal cord itself is becoming damaged by being compressed due to spinal canal stenosis leading. Laminectomy can be a very effective way of decompressing the spinal cord to prevent further damaging from occurring.
Other indications include conditions that require surgical access to the spinal canal, for example, removal of spinal tumours, treating abnormal fluid collections, detethering the spinal cord, treating certain types of spinal injuries, and treating certain vascular conditions of the spine.
After surgery the recover depends to some degree on the extent of the laminectomy involved, but as a general rule the procedure is well tolerated with people remaining in hospital for usually a couple of nights and getting back into doing things over the two to four weeks after discharge.

Recovery will also depend on the underlying condition.
For example, in the most common situation where this operation has been needed for spinal cord decompression a patient’s recovery will be influenced by the degree of spinal cord damage that they had already sustained prior to having surgery.
Cervical Laminoplasty
This is similar to cervical laminectomy in that in involves an operation on the back of the neck to treat conditions inside the spinal canal. The main difference is that unlike laminectomy in which the lamina is removed laminoplasty involves replacing this bone (e.g. if there is no stenosis and the surgery was done to remove a tumour from within the spinal canal) or altering the shape in some way to increase the overall dimension in some way. In some situations it may offer an alternative to cervical laminectomy alone or cervical laminectomy and fusion.
Posterior Cervical fusion surgery and spinal stability
Spinal fusion refers to the joining up of one bone in the spine to another. It often involves a combination of placing internal fixation or “instrumentation” (e.g. screws, rods, or plates) and bone grafting (either bone taken from the spine or somewhere else in the body, or bone graft “substitutes” that function in a similar way). The purpose of the instrumentation is to achieve immediate stability by holding the bones together in a solid fashion, while the bone grafting allows the process of healing by fusion to proceed over the coming months. This process is very similar to fixing a broken bone where some form of hardware may be needed to immobilise the fracture while the body then heals the break over time.
The goal of spinal fusion is to provide the spine with the stability it needs that it may have lost as a result of the particular disease or condition requiring treatment. The concept of “stability” is best defined of the ability of the spine to do its job, which in turn is generally understood to mean the ability to protect the spinal cord and nerves, to allow a solid basis for movement across the body, and to do so while also minimising the possibility of long term pain or deformity. Certain conditions or injuries can compromise the ability of the spine to perform this function, and we refer to this as the spine having become “unstable”. In some situations this may lead to excessive or abnormal motion or alignment between one level of the spine and another, and these so called “dynamic” factors may contribute to the problem that ends up needing an operation to treat. As part of the goal of the surgery in these situations spinal fusion may be necessary to re-establish the stability of the spine, to re-align and correct deformity, and to prevent further injury from these uncontrolled dynamic forces.
Fusion for its own sake has rightly developed a controversial name in surgery mostly due to attempts in treating so-called axial spinal pain (neck or back pain WITHOUT nerve compression) where success rates are difficult to predict. However, in other situations fusion may be an important component of treating conditions that have led to the spine developing instability (e.g. injuries, arthritis, infections, tumours etc), or in order to reconstruct the spine after surgery done to decompress the spinal cord or nerves (usually performed at the same time).
Recovery from fusion surgery can take a little longer than from decompression surgery alone but very much depends on the extent of the dynamic factors or deformity that is being addressed (i.e. how many levels need to be treated, which part of the spine is involved, and whether there are confounding medical problems such as osteoporosis, excessive obesity, diabetes, etc). In some cases a period of planned rehabilitation or convalescence in a dedicated rehabilitation hospital under the care of a rehab physician may be beneficial as an interval step in the recovery process between leaving the acute care surgical hospital and before going home for further out-patient based physiotherapy etc.
Spinal stability is then obtained by reconstructing the discectomy site with a variety of implants such as cages or plates, depending on the details for the individual case. These implants provide immediate stability of the spine and promote fusion to occur as part of the healing process over the weeks and months ahead.
Since the lion share of day to day neck movement occurs at the top two levels (i.e. between the bottom of the skull and C1, and between C1 and C2) fusion of one or even more of the levels below this results in very little if any decrease in functional movement in the neck. The individual levels involved no longer move but the other levels in the spine accommodate so that people get back to all normal activities. In specific cases professional sports players have even returned to high impact sports such as first grade rugby league once they have recovered from this operation indicating how robust the reconstruction of the spinal stability can be with this procedure.
Generally patients will be in hospital for one to two nights with the remainder of the recovery period very similar to microdiscectomy. This procedure is usually well tolerated with any postoperative discomfort usually similar to a cold or laryngitis with sore throat, minor hoarse voice, and some minor temporary discomfort when swallowing.
Cervical Disc Replacement (disc arthroplasty)
Like anterior cervical fusion this operation involves an approach to the spine via a small incision on the front of the neck in order to remove a disc so as to decompress the spinal cord or spinal nerves. Unlike fusion however the purpose of a disc arthroplasty is to maintain motion by replacing the disc with an artificial one. By maintaining motion across the individual spinal segment the hope is that this may reduce the likelihood of so-called adjacent level disc disease.
This process refers to a specific situation that may result after an anterior spinal fusion. The motion segments above and below a fusion can be placed under greater mechanical stress due to the mismatch in stiffness between the fused segment and its adjacent still moving neighbours. Over time, this additional stress may aggravate the development of spondylosis or disc herniation in these adjacent segments over and above the background level at which these conditions would have occurred on their own due to wear and tear. The goal of motion preservation is to try and avoid this by reducing the mismatch in elasticity between the treated segment and the adjacent ones.
Many studies now show that disc arthroplasty can be an effective treatment when compared to anterior cervical fusion. However, some controversies still remain and continue to divide opinion. Some of these relate to the somewhat short follow up to date and the unknown as to what may happen to the moving device over many years or decades of life and what this may mean for the patient’s neck. Furthermore, the type of motion that is preserved is not exactly the same as the motion that existed initially and so this somewhat “abnormal” motion may lead to a different pattern of loading of the joints with increased wear and tear that may cause trouble in the future. Other debated issues include unique setbacks that may result due to the nature of the implanted materials over time (such as metal wear or bone resorption at the arthroplasty-bone interface), and the possibility of certain cognitive biases within the literature that confound interpretation of these studies.
If a disc arthroplasty develops any of these problems the fall back solution is usually to revise the procedure and perform an anterior fusion due to its much longer track record in surgery and well identified role in maintaining spinal stability.
Anterior Cervical Decompression and Fusion
This procedure is performed in the neck and may be necessary to decompress the spinal cord and reconstruct the stability of the spine in certain cases. A small incision is made on the front of the neck usually within an existing skin crease. A natural corridor exists in the body between the throat on one side and the carotid artery and its sheath on the other. This corridor is developed which allows direct access to the front of the vertebral column in the neck without the need to dissect any other tissues. Once the spine is reached an xray is taken to correctly identify the level involved and specialised equipment is placed to maintain the exposure. Using an operating microscope the abnormal disc and bone spurs can then be removed and by doing so the spinal cord and nerve root decompressed.



