Tumours
Compared to the much more common degenerative conditions or injuries such as spondylotic spinal canal stenosis or intervertebral disc herniation tumours of the spine a relatively rare but potentially very serious condition that may require surgery.
Amongst the tumours the most common involve the bones of the spine directly, especially “metastases” from those cancers which have started elsewhere and spread to the spinal bones via the blood stream. This may occur with conditions such as lung, kidney, breast, or prostate cancer. Treatment will often require a so-called “multi-disciplinary” approach with expertise from cancer specialist (medical oncology and radiation oncology) as well as spinal surgery. Similarly, tumours of the blood such as multiple myeloma and plasmocytoma can occur in any bone of the body and therefore may turn up in the spine. Once again a multi-disciplinary and targeted treatment approach is needed with haematology (specialists in diseases of the blood), oncology and surgical input.
Thankfully, the more common tumours of the spinal canal itself tend to be benign. These include schwannoma (and less commonly neurofibroma) which arise from the lining cells of the spinal nerves, and meningioma which arises from the dura (the tissue which surrounds and contains all of the structures within the spinal canal) or cells attached to the dura. Unfortunately, benign doesn’t always mean “safe” – although these tumours are usually not cancerous they can however continue to grow and take up more and more space at the expense of the spinal cord or nerve roots, potentially leading to damage to these structures. Treatment options for these lesions include observation, surgery, or radiotherapy depending on their size, how quickly they seem to be growing, the extent to which they may already be causing spinal cord or nerve damage, etc. Surgery for these tumours requires the delicacy of microneurosurgery but fortunately for the majority of these tumours gross total resection by surgery is often curative.
Least common of all are those tumours which occur within the substance of the spinal cord itself or arise from the various supportive tissues that line the spinal cord. Some of these can be more aggressive such as astrocytoma and ependymoma and may require combinations of treatment such as surgery and radiotherapy. Others tend to be more common in children or young adults such as juvenile pilocytic astrocytoma and may not grow as rapidly as those occurring in later life. Yet others are benign and curable with surgical excision such as hemangioblastoma and cavernous haemangioma. Again, benign in this context doesn’t always mean safe in that even these benign lesions may lead to paralysis if not treated. Clearly, this surgery is very delicate and should only be done by highly trained neurosurgeons.
A careful and thorough work up is required both within the spine and outside the spine to come up with the appropriate treatment options in each individual case, often needing a number of visits and consultation with experts in other disciplines through multi-disciplinary team case conferences.

Vascular Lesions
A number of vascular lesions can occur in the spine although generally they are rare. A multimodality response between surgery and interventional neuroradiology may be required to identify the exact problem and determine the best treatment. In addition to standard imaging such as MRI scan patients may need a specialised form of test known as a spinal angiogram to fully identify the diagnosis.
Depending on the type of lesion treatment options may involve observation, embolization (whereby the angiogram is used to inject various materials to block off the lesion from the inside), surgery, or some combination of all.
Trauma
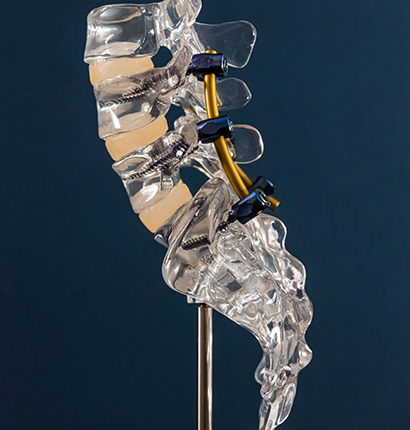
Spinal fractures can result when the forces across spine exceed the ability of the spine to withstand them. This can occur if either the forces are too strong (such as in a fall from a height or in a motor vehicle accident) or if the strength of the spine is reduced (e.g. due to osteoporosis, tumour, or some other disease process of the bone). A fracture that occurs due to a fundamental weakness of the bone is sometimes referred to as a pathological fracture.
The treatment of spine fractures needs to take into account all of these so-called biomechanical factors, as well as those related to the individual patient’s expectations, age, and general state of health. Depending on the case there may be different options available ranging from reassurance, wearing a brace or collar, augmentation of the bone with cement, or surgical reconstruction often involving some form of instrumented fusion. A careful assessment of all these issues is required to determine the best option in the individual case.
Spinal deformity
Deformity refers to the spine not having the usual or “normal” general shape and alignment. This can be as a result of the way things developed from birth, the wear and tear changes that occur as part of the process of spondylosis, the result of instability due to previous injury, or certain diseases that may affect the spine or the spine muscles.
In many situations any deformity is more of an Xray issue than a real one meaning that people can quite happily co-exist with a spine that may not have the original or textbook alignment. In other situations however deformity may lead to chronic pain or nerve tissue entrapment. In yet others the need to treat one condition of the spine may affect the possibility of developing further deformity or trouble in the future. A careful assessment of the clinical and radiological features is required to make an appropriate judgement of what if anything should be done.
Scoliosis refers to a curve in the spine seen from front on (or in the so-called “coronal plane”). Surgery to “correct” a scoliosis can on occasion be quite extensive and in some cases there are controversies as to how much should be done.
Change in the normal curves in the spine seen from side on (the so-called “sagittal plane”) may be described by the straightening or loss of those normal curves in the initial stages and then by the development of abnormal curves as the deformity progresses. For example, it is not uncommon in the cervical spine in the neck for the process of spondylosis to result over time in a general forward bending of the spinal column such that, initially, as it becomes straighter it may be said to have undergone “loss of lordosis” and then, as the process progresses and forward bending develops, it can be describes as having developed “kyphosis”. These changes may amplify the effects of spinal stenosis leading to nerve or cord compression and therefore it may be necessary to address or anticipate the impact of deformity when planning treatment.
All of these changes will affect as the spine moves and will interact with other parts of the spine in the overall concept of “spinal balance”. This is the principle whereby the body weight is supported comfortably above the pelvis without being thrown too far forward or too far backward off the pivot point. For example, an exaggerated thoracic kyphosis due to aging and osteoporosis which would tend to through the body weight forward may result in “compensatory” increases in lordosis of the cervical and/or lumbar spine to bring the overall vertebral column back into balance. If balance cannot be maintained it may in some situations lead to difficulties such as pain, trouble with standing and walking, or nerve or spinal cord compression.
Surgery for spinal deformity usually requires some form of reconstructive fusion and careful assessment in order to know when something needs to be done, and when reconstruction is required to look for a solution that ideally involves doing enough without doing too much.
Risk factor modification and preventative measures
Although the condition of spondylosis is in part an unavoidable aging process of the spine that will occur in all of us there are some risk factors which are generally understood to contribute to the extent and speed at which it develops. Some of these risk factors are beyond our control such as genetic predisposition, hereditary conditions, the suffering of previous injuries, etc. Research on stem cell therapy offers some hope that in the future some of these issues may be able to be addressed.
However, other risk factors are potentially able to be modified now to reduce the impact of spondylosis and, if you like, ensure your spine will last as long as you do. Broadly these risk factors include:
Giving up smoking – smoking “ages” the body tissues prematurely which is one reason why long term smoking can lead to grey, wrinkly skin and listless hair etc. In the spine this may aggravate the dehydration and breakdown of the discs and cartilages.
Identification and correction of errors or posture – how we sit, stand, and position our necks and backs during activities and work can over the years lead to “hot spots” of degenerative changes that may become symptomatic. Avoiding these postural errors may help reduce the extent to which these form.
Reducing weight and keeping weight down – in a common sense way the heavier we are the more load and stress there is across the spine as we go about our day in the upright position. Even when sitting down and seemingly resting our spine is working to support our bodies against gravity. Cartilage and disc wearing occurs as a direct response to the day by day and year by year loading that occurs based on our unique upright human physiology. Avoiding or reducing excessive weight gain can reduce these forces over time.
Avoiding wherever possible “injury prone activities” – this is particularly the case for the lumbar spine where the discs can be exposed to significant torsional loading moments in activities that involve repetitive bending, lifting, and twisting movements. These can be amplified in those activities that involve a lift, twist, and put down type action across the spine. Over time this may lead to so-called “micro-injuries” in the discs resulting in tears and sometimes frank herniations.
Core strengthening exercises – bones, cartilages, and ligaments will to some degree always wear down over time. However, with exercise we can maintain the strength in our muscles to help off load the forces that our spines are exposed during day to day activities. The so-called “core muscles” are those in the back and neck itself and also in the trunk generally such as the stomach muscles which, among other things, function to help spread the load that occurs through our spine and trunk as we go about our lives. The stronger they are the more that can be done with safety. Conversely, if core strength is allowed to lapse then all of the forces that occur must be met by the spine alone and hence it is more likely to suffer wear and tear injuries. In a very real sense therefore it is important to put the effort in to age well. Nonetheless, exercise carries the risk of injury and so it is worthwhile speaking to a physiotherapist or exercise physiologist to ensure that the these exercises are being down in an appropriate way for your individual case and with proper technique (a small error in technique for example may have the unwanted consequence of an injury prone activity as described above).
It can sometimes be helpful to remember that our spine evolved over hundreds of millions of years and became a major point of difference between humans and other mammals allowing us to walk around in an upright position. Furthermore, evolutionary anatomy teaches us that we separated from our closest primate cousins (chimpanzees) roughly 6 million years ago with our ancestors leaving the forests and becoming long distance runners on the African savannah. Modern humans started life in this habitat perhaps 700 thousand years ago. However, in only the last few hundred years we have developed an increasingly sedentary life style with even the most active of us still somewhat more stationary than our evolutionary forebears. A great deal of the trouble that people can experience in their spines comes from this mismatch between what our bodies evolved to do and what we actually do. Many measures aimed to improve spinal health come about by recognising this difference and trying to minimise it by becoming less sedentary and more active.
Axial Spinal Pain (low back pain and neck pain)
Spinal pain and particularly low back pain is a very common problem with as many as seventy percent of the adult population likely to experience at least one episode of significant low back pain in their lives. For most this is a self limiting problem that gets better, and as such it is so common that it can almost be considered as part of life in modern human societies rather than a sign of something going wrong. For others however it can persist or and become a chronic and disabling condition that may prevent normal activities and work, and yet others may be prone to multiple flare ups over their life in an on again off again pattern.
The initial treatment of acute low back pain usually involves a period of rest with simple pain killers (such as paracetamol or anti-inflammatories) followed by gentle mobilisation and physical therapies. Physiotherapy, osteopathy, chiropractic therapy, and various combinations of these can be tried together with other alternative strategies such as acupuncture. Stronger medications carry very real risks of dependence and aggravating the pain system in the body and so generally need to be avoided.
Medical therapies usually revolve around rehabilitation programmes, exercise related treatment, and core strengthening training. There can sometimes be a role for injection based therapy (e.g. cortisone injections).
The fact that there are so many treatment options that get tried for low back pain highlights one of the main dilemmas in this condition, i.e. the difficulty in diagnosing the underlying cause of the pain and the lack of knowledge in medicine as to the correct treatment. Even modern test such as MRI and nuclear scans may not reliably show the exact generator of the pain and often get mis-interpreted in this “grey area” of medicine.
Nonetheless, for pain that is persisting despite initial treatment, pain that is getting worse with unusual features (such as waking someone at night), or pain that has any flavour of nerve compression such as spreading down the legs an MRI is usually required to exclude identifiable causes such as nerve compression, fractures, deformity, tumours, etc. If these conditions are excluded however the MRI may not be able to show the underlying cause of pain in axial spinal low back pain.
Surgery therefore has a somewhat guarded and controversial role in treating this condition. Even experienced spine surgeons may hold divided opinions as to how effective surgery may or may not be in trying to treat low back pain alone. It requires a nuanced and careful assessment of the case, and sometimes the best thing a surgeon can do is to advise where surgery is just not a good option.



